Ourhealthhistory - Hello, lovely readers! How are you? Today, we delve into the fascinating topic of pelvic changes after childbirth. It's a subject that many new mothers may be curious about, and we're here to provide you with the medical explanation you've been seeking.
Pregnancy and childbirth bring about significant transformations in a woman's body, and understanding these changes is essential for postpartum recovery and overall well-being. So, let's embark on this enlightening journey together, exploring the intricacies of pelvic changes after childbirth. Please continue reading to uncover the valuable insights that await you.
Introduction to Pelvic Changes After Childbirth
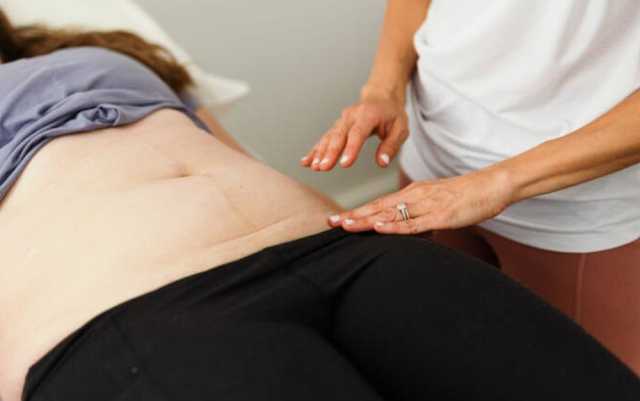
After childbirth, a woman's body undergoes remarkable changes, particularly in the pelvic region. The pelvic floor muscles, which provide support to the bladder, uterus, and bowel, may become weakened or stretched during labor.
This can lead to issues such as urinary incontinence and pelvic organ prolapse. Furthermore, the pelvic bones may also experience changes due to the pressure exerted during delivery. These changes can impact a woman's overall well-being and quality of life.
It's important for new mothers to be aware of these changes and seek appropriate postnatal care to address any issues that may arise.
Understanding the Female Pelvic Floor
The female pelvic floor refers to a group of muscles, ligaments, and connective tissues that support the pelvic organs, including the bladder, uterus, and rectum. Understanding the female pelvic floor is crucial for maintaining overall health and well-being.
These muscles play a key role in urinary and bowel control, sexual function, and supporting the growing fetus during pregnancy. Factors such as pregnancy, childbirth, aging, and high-impact activities can weaken the pelvic floor, leading to issues such as incontinence and pelvic organ prolapse.
Awareness of the pelvic floor and its importance can help women take proactive steps to maintain its strength and function, promoting better long-term health.
Hormonal Changes and their Impact on the Pelvic Floor
Hormonal changes can have a significant impact on the pelvic floor. During menopause, decreased estrogen levels can lead to weakening of the pelvic floor muscles, contributing to issues such as urinary incontinence and pelvic organ prolapse.
On the other hand, during pregnancy, increased levels of relaxin hormone can soften the ligaments and muscles in the pelvic area, preparing the body for childbirth but also potentially leading to pelvic instability.
Additionally, hormonal fluctuations during the menstrual cycle can affect pelvic floor function, with some women experiencing increased symptoms of pelvic floor disorders during certain phases. Understanding the influence of hormones on the pelvic floor is crucial for developing targeted interventions and treatments to address these issues.
The Role of Pregnancy in Pelvic Floor Changes
Pregnancy plays a significant role in causing changes to the pelvic floor. The weight of the growing fetus puts pressure on the pelvic floor muscles and ligaments, leading to stretching and potential weakening.
Hormonal changes during pregnancy also contribute to the relaxation of connective tissues in the pelvic area. As a result, many women experience pelvic floor issues such as urinary incontinence and pelvic organ prolapse during or after pregnancy.
It's important for expectant mothers to be aware of these potential changes and to engage in pelvic floor exercises to help maintain strength and function. Additionally, seeking guidance from healthcare providers can aid in managing and addressing any pelvic floor concerns that may arise during pregnancy and postpartum.
Vaginal Delivery and its Effects on the Pelvic Floor
Vaginal delivery is a common method of childbirth that has both short-term and long-term effects on the pelvic floor. During delivery, the pelvic floor muscles and tissues undergo significant stretching and pressure as the baby passes through the birth canal.
This can lead to temporary weakening and stretching of the pelvic floor, resulting in symptoms such as urinary incontinence, pelvic organ prolapse, and sexual dysfunction. However, the majority of women recover from these symptoms within the first few months postpartum.
Nonetheless, some women may experience long-term effects, such as persistent urinary incontinence or pelvic organ prolapse, which may require further medical intervention. It is important for women to be aware of the potential effects of vaginal delivery on their pelvic floor and to seek appropriate care and support during the postpartum period.
Healthcare professionals can provide guidance and exercises to strengthen the pelvic floor and help prevent or manage any potential complications.
Cesarean Section and Pelvic Floor Changes
A cesarean section, commonly referred to as a C-section, is a surgical procedure used to deliver a baby. It involves making an incision in the mother's abdomen and uterus to remove the baby. While C-sections are often necessary for medical reasons, they can have an impact on the pelvic floor.
The pelvic floor is a group of muscles that support the organs in the pelvis, including the bladder, uterus, and rectum. During a C-section, these muscles can be weakened or damaged. This can lead to issues such as urinary incontinence, pelvic organ prolapse, and sexual dysfunction.
To prevent or minimize these complications, it is important for women who have had a C-section to engage in pelvic floor exercises, also known as Kegel exercises. These exercises help strengthen the pelvic floor muscles and improve their function.
Additionally, women should consult with their healthcare provider for further guidance and support in managing any pelvic floor changes after a C-section. Overall, while a C-section can be a life-saving procedure, it is essential for women to be aware of and address the potential pelvic floor changes that may occur as a result.
Pelvic Organ Prolapse: Causes and Risk Factors
Pelvic organ prolapse occurs when one or more pelvic organs, such as the uterus, bladder, or rectum, descend from their normal position and bulge into the vaginal canal. This condition affects millions of women worldwide and can significantly impact their quality of life.
Several factors contribute to the development of pelvic organ prolapse, including pregnancy, childbirth, age, obesity, chronic constipation, and menopause. During pregnancy and childbirth, the pelvic floor muscles and ligaments may weaken or stretch, increasing the risk of organ prolapse later in life.
Age and hormonal changes during menopause also play a role in weakening the pelvic floor support. Obesity and chronic constipation can further strain the pelvic floor, making prolapse more likely. It is important for women to be aware of these causes and risk factors to take preventive measures and seek appropriate medical care when needed.
Early diagnosis and treatment can help manage symptoms and improve overall well-being.
Urinary Incontinence Post Childbirth: A Common Concern
Urinary incontinence, also known as bladder leakage, is a common concern experienced by many women after childbirth. This condition occurs when there is involuntary leakage of urine, which can be triggered by activities such as coughing, sneezing, or even laughing.
The pelvic floor muscles, which support the bladder and control urine flow, can become weakened during pregnancy and childbirth, leading to urinary incontinence.Postpartum urinary incontinence can be distressing and affect a woman's quality of life.
It can cause embarrassment, self-consciousness, and can even lead to social isolation. Many women feel hesitant to seek help or discuss their symptoms due to the stigma surrounding this issue. However, it's important to remember that urinary incontinence is a common and treatable condition.
There are various treatment options available for urinary incontinence post childbirth. Pelvic floor exercises, also known as Kegel exercises, are often recommended as a first-line treatment. These exercises involve contracting and relaxing the pelvic floor muscles to improve their strength and coordination.
Additionally, lifestyle modifications, such as maintaining a healthy weight, avoiding caffeine and alcohol, and practicing good toilet habits, can also help manage urinary incontinence.In some cases, medical interventions may be necessary.
These can include medications that help control bladder function or surgical procedures to repair or support the pelvic floor muscles. It's important to consult with a healthcare professional to determine the most appropriate treatment plan based on individual needs and circumstances.
Remember, you are not alone in experiencing urinary incontinence after childbirth. It's a common condition that can be effectively managed with the right approach. Seeking help and support from healthcare professionals, as well as connecting with other women who have gone through similar experiences, can make a significant difference in managing and improving the quality of life for those affected by postpartum urinary incontinence.
If you have any concerns or questions regarding urinary incontinence after childbirth, it's recommended to reach out to a healthcare professional for guidance and support. They can provide personalized advice and develop a treatment plan tailored to your specific needs. (Ourhealthhistory/Admin)


Posting Komentar
0Komentar